January 1, 2014
Sheku Kamara, director of the Rapid Prototyping Consortium at the Milwaukee School of Engineering, says he believes additive manufacturing (AM)—better known as 3D printing in mainstream discussions—is “made for the medical industry.”
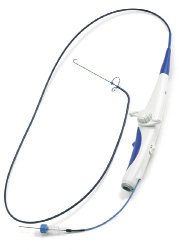 When Ablation Frontiers, a medical device company, urgently needed several hundred Ablation tools for a trade show, it turned to RedEye to produce them in additive manufacturing. |
Whereas traditional manufacturing methods are ideal for high-volume production of parts with standard geometric features, AM can produce one-of-a-kind models of complex organic shapes in low volume. The growing use of pre-surgical models—3D-printed physical replicas of the cross-sections that must go under the knife—is a relatively new trend made possible by AM’s ability to speedily produce single units for one-time use, custom-built from the CT scans of target patients.
The Consortium’s rapid prototyping hardware setup includes iPro8000, SLA-3500 and Sinterstation 2500plus from 3D Systems; Fortus eT from Stratasys; and Spectrum Z510 from 3D Systems (previously a Z Corp brand, acquired by 3D Systems). Its members are industry-leading names in the medical sector: Johnson & Johnson, Baxter Healthcare, and Zoetis (formerly Pfizer Animal Health), to name but a few.
By Kamara’s conservative estimate, more than 50% of the Consortium members own and operate their own rapid-prototyping facilities, deploying inexpensive concept-model printers to high-end machines. But the interest, R&D activities and technology acquisitions only began to pick up in the last four or five years, he notes. The insiders aren’t publicizing what they’re doing with AM because, he says, “it’s a competitive advantage for them.”
Who Gets the Bill?
In automotive and aerospace sectors, manufacturers are increasingly relying on digital mockups and simulation software to circumvent the cost of building and crashing physical prototypes for safety tests. But in the medical sector, tangible 3D-printed models are giving surgeons and physicians an option they’d never had before: the ability to practice and plan computer-guided surgery on a mockup of their patient’s anatomy.
In October 2013, DePuy Synthes CMF (craniomaxillofacial), a division of Johnson & Johnson, launched a new offering called TRUMATCH CMF. It’s a pre-operation planning service for facial reconstruction, orthognathic surgery, distraction and cranial reconstruction. Much of it is powered by AM, according to the company. As the press release explains: “A digital file is translated into a physical object by a 3D printer to create patient-specific surgical guides and occlusal splints. This enables transfer of the pre-operative plan to the operating room, potentially reducing OR time and assisting in the placement of implants.”
 |
 |
| In the development of a new device to treat benign prostatic hyperplasia (left), Kablooe Design needed seven to 10 design iterations for testing. The company relied on RedEye’s on-demand rapid prototyping services to create functional prototypes, shown here as 3D renderings (right). | |
Kamara observes that the ability to print out the target region for surgery, with all the nerves and blood vessels in color, and to see where the veins are connected is absolutely huge. “But how can that be quantified?” he asks. “That’s the challenge.” To put it bluntly, who would pay for the print job? At least for now, the question produces more debates than answers.
Bridging Engineering and Life Sciences
Jean Colombel, vice president of life sciences industry for Dassault Systemes, says he believes the medical device industry can benefit from greater collaboration between engineers and physicians, who often speak different languages and use different lingos. (For more on this, read “From Classical Mechanics to Biomechanics,” July 2013.)
“The knowledge about human beings and human bodies is still a partial knowledge,” he says. “How can we get the expertise of the physicians and the case histories of their patients added to the ideas of the engineers? It’s really about getting them to collaborate more, so they can create digital models for simulation.”
According to Colombel, Dassault’s SolidWorks 3D mechanical software is “a leading 3D design tool for the medical device industry.” He predicts that “leveraging 3D as part of medical community will improve communication between doctors and engineers.”
Even though Dassault is primarily a software powerhouse, the company keeps a mini-manufacturing center called FabLabs on its Paris campus. Among the hardware choices at the facility is a pair of Cubify 3D printers from 3D Systems. Priced at $1,299, they target home users and hobbyists with limited CAD software expertise.
The Missing Software
In aerospace, automotive and consumer goods manufacturing, the current crop of mechanical 3D modeling packages serve as concept modelers. But the range of geometry you can produce in them may prove inadequate to address the non-uniform, asymmetrical anatomical shapes medical professionals need to analyze.
“In my opinion, the software is lagging—not just in medical application, but even in consumer goods,” says the Consortium’s Kamara. “In 3D printing, I can print anything. Shape complexity is an advantage. But not so in most of CAD software.”
Detailed humanoid shapes are the domains of high-end character modeling and animation programs like Autodesk Maya, the standard tool for filmmakers and game developers. But the learning curve for such a program may prove too steep even for regular 3D software users. It would certainly be an unfair burden on medical professionals, whose primary job function is not 3D modeling.
At the Consortium, students use Mimics from Materialise and Freeform Plus from Geomagic (a subsidiary of the rapid prototyping machine maker 3D Systems). Both packages offer one crucial function for medical application: You can sculpt 3D models out of CT, MRI and ultrasound data.
From Prototype to Production
Most people consider AM to be a prototyping technology, suitable for creating test models and mockups, not for full production run. But RedEye, a division of Stratasys, defies this generally accepted belief. Medical device projects account for about 15% of RedEye’s business, according to Jeff Hanson, RedEye’s manager for business development.
“Typically, medical companies come to our portal ]website] at the prototyping phase,” Hanson says. “Our job is to understand the story of the part: What’s the end use, the intended manufacturing material, the market? If we know those, we might be able to migrate the customer from prototyping to manufacturing.”
In medical device manufacturing, early digital concepts are likely to go through many iterations. Some are minor geometry adjustments; others are more drastic to improve the instrument’s performance. They’re often prompted by findings from lab tests, cadaver tests and clinical trials.
“If ]the customer] comes to us during an early concept phase, everything is at risk for change,” notes Hanson. “Maybe the strain release doesn’t work right, a boss interferes with the device’s operation, or the skin doesn’t fit—these are typical design changes.”
For large-volume production of devices that measure bigger than the built chamber of a 3D printer, traditional manufacturing methods are still the better choice. But RedEye has found a niche in low-volume, quick-turnaround production runs, described by Hanson as “in the low thousands.” Often, on-demand 3D printing like RedEye’s services can be the best way to introduce a new product to the market without committing to costly machine and mold setups.
Work in Progress
The U.S. Food & Drug Administration (FDA) and other regulatory bodies insist on compliance, not just with the medical devices manufactured, but also with the manufacturing processes themselves. To be certified for medical use, the way the machine cures print materials itself is subject to close examination.
3D printer makers have done an admirable job developing print materials that are acceptable for medical use. The Consortium’s Kamara points to the development of polyetherketoneketone (PEKK) polymer, a medical-grade material that can be used with 3D printing and is acceptable for implants, as an example.
Although complying with stringent regulatory requirements like ensuring a sterilized manufacturing environment for implants created in 3D printers is a work in progress, late-breaking news shows encouraging signs. In November, polymer-based cranial implants made with the AM process from EOS became the first of its kind to receive FDA’s 510K clearance.
Tom Weisel, president of medical device developer Arch Day Design, states that he and his team “print instruments and occasionally anatomical parts such as bone sections. It will be nice when the ]3D-printing] materials represent bone more accurately.” That would allow them to print, for instance, “a bone with cancellous and cortical sections.”
How soon will Weisel’s wish become a reality? That may depend on how big a chunk of the AM market’s revenues the medical sector is hauling in. “We can’t put in the R&D effort on such materials until we know a return on the investment,” explains RedEye’s Hanson. “We usually wait until the market demand reaches a certain point.”
For the medical industry that has already discovered 3D printing, it’s difficult to ignore the advantages the technology offers. As the Consortium’s Kamara concludes, “If a picture is worth a thousand words, a prototype is worth a thousand pictures.”
Kenneth Wong is Desktop Engineering’s resident blogger and senior editor. Email him at [email protected] or share your thoughts on this article at deskeng.com/facebook.
More Info
Subscribe to our FREE magazine, FREE email newsletters or both!
About the Author
Kenneth Wong is Digital Engineering’s resident blogger and senior editor. Email him at [email protected] or share your thoughts on this article at digitaleng.news/facebook.
Follow DE